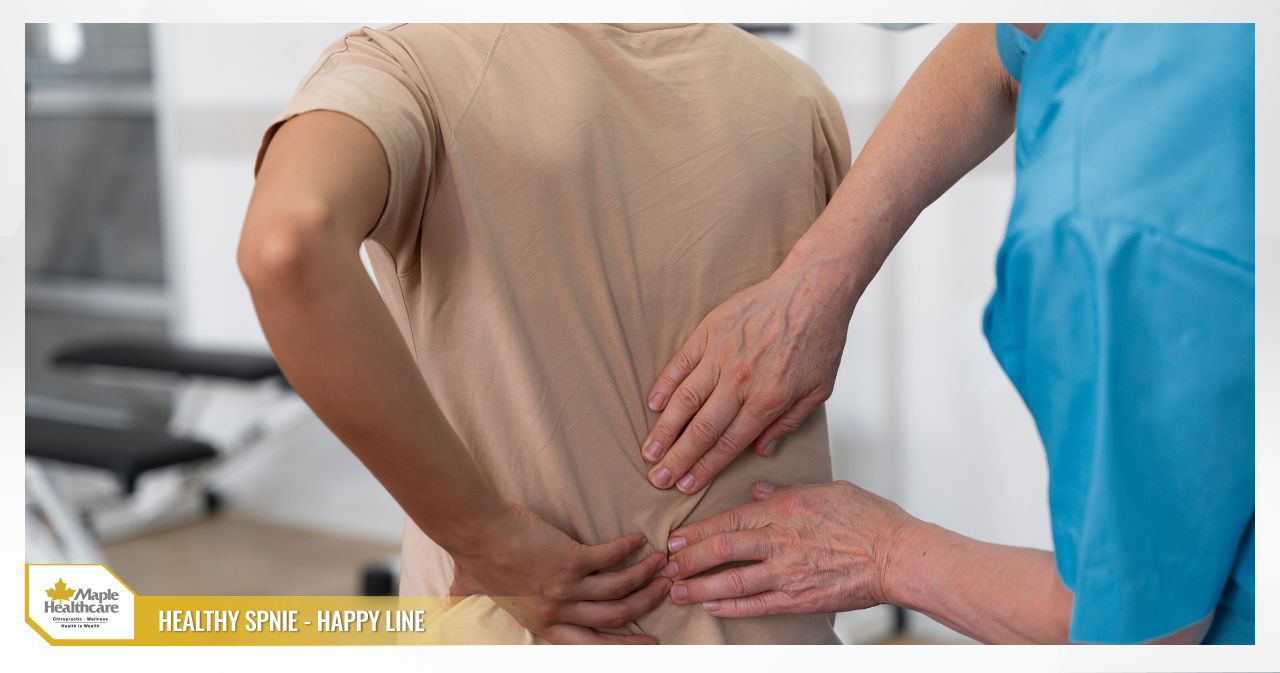
How Dangerous Are the Complications of Spinal Degeneration, and How Can They Be Prevented?
Complications of spinal degeneration are a top concern for anyone facing persistent back pain and neck stiffness. Spinal degeneration is not just a natural part of aging; it’s a functional decline of the intervertebral discs, joints, and ligaments, leading to the formation of bone spurs. If not addressed and managed properly, this condition can progress to serious complications such as numbness and tingling in the limbs, herniated discs, compression of nerve roots and the spinal cord, and even paralysis or disability.
More alarmingly, spinal degeneration and its consequences are increasingly affecting younger people, appearing even in young adults due to improper lifestyle and work habits.
This article was prepared by the team at Maple Healthcare in Ho Chi Minh City to give you a comprehensive and easy-to-understand overview of the signs of spinal degeneration and the dangerous complications that can occur. By reading this article, you will learn how to:
- Recognize the early warning signs.
- Understand the level of risk to avoid the potential for disability.
- Grasp an effective prevention and treatment roadmap, starting with small changes in your daily life.
We will explain everything systematically, along with specific, practical guidance so you can proactively protect your spinal health.
What Is Spinal Degeneration and How Do Complications Arise?
To understand the complications, we first need to grasp what spinal degeneration is. It is a complex degenerative process in the spine that includes:
- Disc Dehydration: The intervertebral discs act as shock absorbers between the vertebrae. As they age or come under excessive pressure, they lose their water content, becoming flatter, drier, and more prone to tearing.
- Facet Joint Wear and Tear: The small joints at the back of the spine (facet joints) experience cartilage erosion, leading to inflammation and pain.
- Ligament Thickening: The ligaments, particularly the ligamentum flavum, become thicker and more fibrous, reducing the spine’s flexibility.
- Bone Spur (Osteophyte) Formation: The body responds to instability by creating small bony growths (bone spurs) around the joints and vertebral bodies.
These structural changes are the source of dangerous complications through the following mechanisms:
- Mechanical Compression:
- Bulging or herniated discs, bone spurs, and thickened ligaments encroach on the space within the spinal canal and the intervertebral foramina (where nerve roots exit).
- The result is compression of the spinal cord or nerve roots, leading to sharp pain, numbness, muscle weakness, and sensory disturbances. This condition is known as spinal stenosis.
- Spinal Instability:
- When the discs and joints weaken, the spine loses its stability. This can cause abnormal micro-movements, which over time can lead to spondylolisthesis (vertebral slippage), spinal deformities (kyphosis, scoliosis), and chronic mechanical pain.
- Chronic Inflammation and Central Sensitization:
- The degenerative process is always accompanied by local inflammation. Constant pain signals are sent to the brain, causing the central nervous system to become hypersensitive. As a result, you may feel more intense and prolonged pain, even when the initial pain trigger is no longer severe.
If early symptoms are ignored, this damage will accumulate and worsen, making treatment much more complex and costly.
Common Complications of Spinal Degeneration
Spinal degeneration can cause a range of health issues that directly impact daily quality of life. Here are the most common complications:
- Chronic back or neck pain: A dull ache lasting more than a month, often with morning stiffness. The pain worsens with strenuous activity, heavy lifting, coughing, or sneezing. This condition can disrupt sleep and interfere with work.
- Herniated disc: This is one of the most common and serious complications. The gel-like nucleus of the disc pushes out through a tear in the outer wall, directly compressing a nerve root or the spinal cord. This causes pain that radiates along the nerve path, numbness, reduced reflexes, and muscle atrophy if left untreated.
- Spinal Stenosis: The spinal canal narrows due to bone spurs, disc herniation, or ligament hypertrophy. In the lumbar spine, it causes sciatica and “neurogenic claudication” (having to stop walking after a short distance due to leg pain and numbness). In the neck, it can compress the spinal cord.
- Cervical Myelopathy: This is a very dangerous complication involving spinal cord compression in the neck. Signs include loss of hand dexterity (difficulty buttoning a shirt, using chopsticks), an unsteady gait, loss of balance, and hyperreflexia.
- Cauda Equina Syndrome: This is a medical emergency. The nerve roots in the lumbosacral region are severely compressed, causing bowel or bladder dysfunction (urinary retention, fecal incontinence), saddle anesthesia (numbness in the area that would contact a saddle), and rapid bilateral leg weakness.
- Spondylolisthesis and Spinal Deformity: Due to instability, vertebrae can slip out of their normal position. Over time, the spine can become deformed, leading to conditions like kyphosis (hunchback) or scoliosis, affecting posture, gait, and appearance.
- Bone spurs causing nerve irritation: Bone spurs can rub against nerve roots, muscles, and ligaments, causing localized pain, especially neck and shoulder pain when turning or tilting the head.
- Osteoporosis and Vertebral Compression Fractures: People with spinal degeneration often move less due to pain, which, combined with age, increases the risk of osteoporosis. Even a minor injury can cause a vertebral compression fracture, leading to acute pain and a loss of height.
- Psychological Impact: Living with chronic pain can lead to insomnia, anxiety, depression, and a significant decline in quality of life.
Classifying Complications by Spinal Location
Depending on the location of the spinal degeneration, complications will present with different characteristic symptoms.
Complications of Cervical Spine (Neck) Degeneration
- Common: Neck pain that radiates to the shoulders and arms, numbness in the fingers, and a weak grip.
- Serious: Cervical myelopathy, as mentioned earlier. Additionally, bone spurs in the cervical spine can compress the vertebral artery, causing symptoms like vertigo, headaches, dizziness, insufficient blood flow to the brain, and vision problems. In rare cases, it can be a risk factor for stroke.
Complications of Thoracic Spine (Mid-Back) Degeneration
- This location is less common but can still occur.
- The main symptom is a dull ache in the mid-back area, with pain increasing during twisting movements and limited ability to bend forward or backward. Cord compression in the thoracic region is very rare but extremely serious if it occurs.
Complications of Lumbar Spine (Low Back) Degeneration
- Common: Dull low back pain, pain radiating down the buttocks and leg along the sciatic nerve path (sciatica), foot weakness (difficulty with tiptoeing or standing on heels), and a limping gait.
- Serious: Spinal stenosis causing neurogenic claudication, and cauda equina syndrome, which can lead to paralysis of both legs if not treated as an emergency.
Severity Levels and Warning Signs
Spinal degeneration can lead to disability or permanent nerve damage if nerve root or spinal cord compression is prolonged. When nerve cells are irreversibly damaged, patients face the risk of limb weakness, loss of sensation, and permanent bowel and bladder dysfunction.
You should see a doctor immediately if you experience any of the following warning signs:
- Severe pain that does not improve with rest or over-the-counter pain relievers.
- Fever, chills, or unexplained weight loss accompanying back pain.
- Pain that worsens at night, waking you from sleep.
- A history of cancer, severe osteoporosis, or long-term steroid use.
- Pain that begins after an injury or accident.
- Signs of spinal cord compression or cauda equina syndrome:
Risk Factors That Increase Complications
Understanding the risk factors helps you be more proactive in prevention. These factors are divided into two groups:
Unmodifiable Risk Factors
- Age: The older you get, the more pronounced the natural degenerative process becomes.
- Genetics: Genetic factors can influence the quality of your cartilage and intervertebral discs.
Modifiable Risk Factors
- Occupation: Jobs that require prolonged sitting, standing, or lifting heavy objects with improper posture.
- Overweight and obesity: This increases the load on the spine, especially the lumbar region.
- Sedentary lifestyle: This weakens the core muscles that support the spine.
- Smoking: Nicotine reduces blood flow to the discs, accelerating the degenerative process.
- Poor posture: Habits like slouching or looking down at your phone place enormous pressure on the cervical and lumbar spine.
- Previous injuries: Past spinal injuries can have long-lasting effects.
- Nutritional deficiencies: A lack of calcium, vitamin D, and other essential minerals for bone and joint health.
The Diagnostic and Evaluation Process for Complications
At Maple Healthcare, the diagnostic process is conducted systematically to accurately determine the cause and extent of the damage:
Clinical Examination
- Medical History: The doctor will ask detailed questions about the location of pain, type of pain, radiation patterns, any numbness/weakness, and factors that worsen or relieve the pain.
- Neuromusculoskeletal Exam: This includes checking the spine’s range of motion, performing specific tests (like the Straight Leg Raise for lumbar nerve compression, or Spurling’s test for cervical issues), and assessing muscle strength, reflexes, sensation, and gait.
- Using Scoring Systems: Pain levels are assessed using the VAS scale (0-10), and the impact on daily activities is measured with functional questionnaires like the ODI (for the back) and NDI (for the neck).
Diagnostic Imaging
- Spinal X-ray: This is a basic method to detect signs like bone spurs, narrowed disc spaces, vertebral slippage, or loss of the natural spinal curve.
- Magnetic Resonance Imaging (Spinal MRI): This is the gold standard for evaluating soft tissues. An MRI clearly shows the condition of the discs (bulging, herniation) and the degree of spinal cord and nerve root compression.
- Computed Tomography (CT scan): Useful for detailed assessment of bone structures, especially in cases of bony spinal stenosis.
Other Tests
- Electromyography (EMG/NCS): Helps determine which nerve roots are affected and the extent of the damage.
- Blood tests: Ordered when inflammation, infection, or other systemic diseases are suspected.
A Guide to Effective At-Home Prevention
“Prevention is better than cure.” Applying the measures below not only helps prevent complications but also slows the progression of the condition.
Maintain Good Posture (Ergonomics)
- When sitting: Always keep your back straight and shoulders relaxed. Your computer screen should be at eye level. Choose a chair with back support that follows the lumbar curve.
- When standing: Distribute your weight evenly on both feet, keeping your ears, shoulders, and hips in a straight line.
- When sleeping: Use a medium-firm mattress and pillow. Sleep on your side with a pillow between your knees or on your back with a pillow under your knees to maintain a neutral spine.
- Move regularly: For every 30-60 minutes of sitting, stand up, walk around, and stretch for 2-5 minutes.
Perform Core and Stretching Exercises
Chin-tuck Exercise
- How to do it: Sit up straight. Slowly pull your chin backward as if making a “double chin,” and hold for 5 seconds.
- Benefit: Strengthens the deep neck muscles, reducing pressure on the cervical spine.
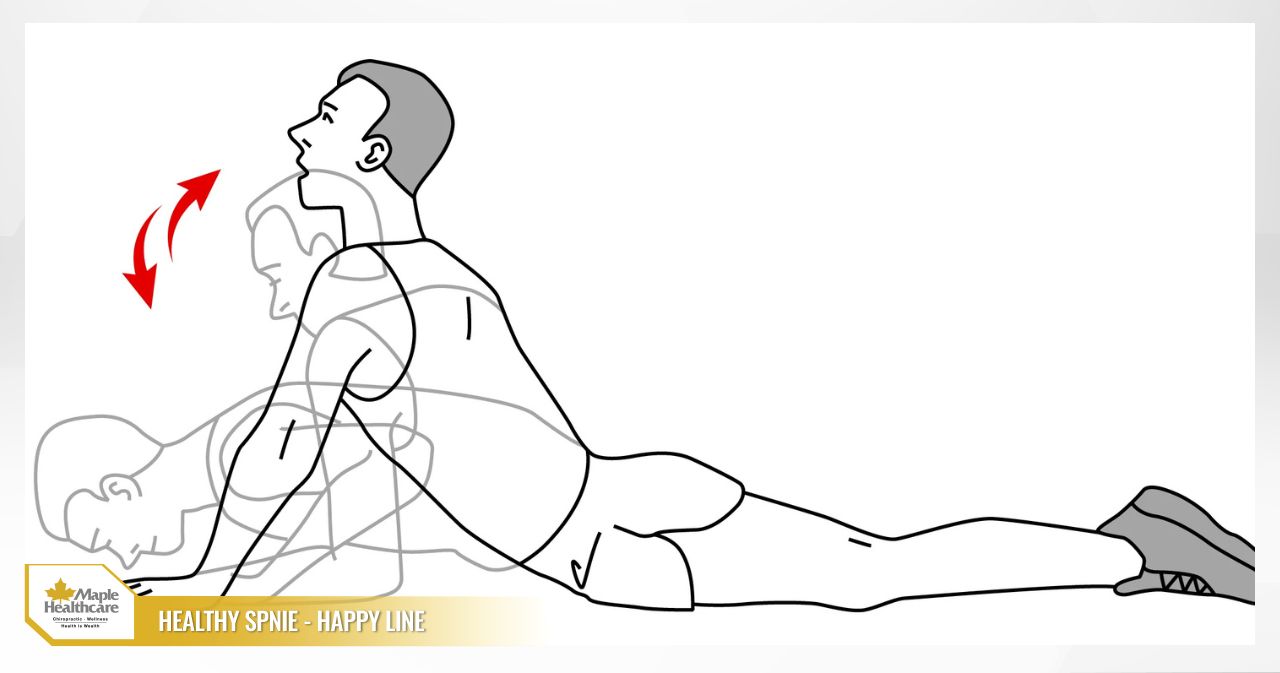
McKenzie Exercise (Prone Press-up)
- How to do it: Lie on your stomach with your hands placed under your shoulders. Slowly straighten your elbows to lift your upper body, keeping your hips and legs on the floor. Hold for 1-2 seconds, then lower down.
- Note: Stop if you feel pain radiating down your legs.
Hamstring Stretch
- How to do it: Lie on your back with one knee bent and the other leg straight. Loop a towel around the bottom of the straight leg and gently pull it toward your chest until you feel a stretch in the back of your thigh. Hold for 20-30 seconds.
Build a Healthy Lifestyle
- Weight management: Lose weight if you are overweight to reduce the load on your spine.
- Quit smoking: This improves blood circulation to nourish the discs.
- Balanced nutrition: Ensure adequate intake of calcium, vitamin D, protein, and Omega-3s from foods like fish, dairy, and green vegetables.
- Regular exercise: Walking, swimming, and yoga are excellent activities for spinal health.
Treatment Methods for Spinal Degeneration and Its Complications
At Maple Healthcare, we prioritize conservative, non-drug, non-surgical treatment methods to address the underlying causes of the condition. The treatment plan is personalized based on the severity and specific complications of each individual.
Mild to Moderate Stage (Self-Care and Conservative Treatment)
- Active Rest: Avoid activities that cause pain but maintain gentle movement.
- Hot/Cold Therapy: Cold packs can help reduce inflammation in the first 48 hours, while heat can help relax muscles and relieve pain afterward.
- Chiropractic Care: Specialized doctors use gentle adjustment techniques to correct spinal misalignments, relieve pressure on nerve roots, improve function, and effectively reduce pain.
- Physiotherapy: Specialists will guide you through specific exercises to strengthen your back and abdominal muscles (core), improve flexibility, and enhance balance. Therapies such as ultrasound, electrical stimulation, and high-intensity laser are also used to reduce pain and promote healing.
More Severe Stage (Medical Interventions)
- Prescription Medication: In some cases, a doctor may prescribe muscle relaxants, anti-inflammatory drugs, or nerve pain medications (gabapentin/pregabalin) for a short period.
- Epidural Steroid Injections: Injecting steroids near the inflamed nerve root area can provide rapid pain relief. This is a temporary solution and should be carefully considered.
- Radiofrequency Ablation (RFA): Uses heat to disable the small nerve branches that cause pain from the facet joints.
When Spinal Surgery Is Necessary
- Indications: Surgery is only considered when there are red flags, progressive neurological weakness, severe pain that does not respond to at least 6-12 weeks of conservative treatment, or significant spinal instability.
- Techniques: Common procedures include decompression surgery (laminectomy, discectomy) to remove the bone or disc material compressing the nerve, which may be combined with spinal fusion if the spine is unstable.
- Note: Surgery always carries risks and requires a long-term rehabilitation process.
When to Seek Immediate Medical Attention to Avoid Dangerous Complications
Do not hesitate. Seek immediate medical attention at a healthcare facility or a specialized clinic like Maple Healthcare if you experience the following emergency situations:
- Signs of cauda equina syndrome: Loss of bladder/bowel control, numbness in the saddle area.
- Sudden and rapidly progressing weakness or paralysis in the legs/arms.
- Severe back pain after a fall or injury.
- Pain accompanied by high fever or unexplained weight loss.
Seeking prompt medical care is key to preventing irreversible nerve damage.
FAQ: Frequently Asked Questions About Spinal Degeneration Complications
1. Can complications from spinal degeneration be completely cured?
Answer: Degenerative damage (like disc dehydration or bone spurs) cannot be completely reversed. However, early and proper treatment can fully manage symptoms, prevent progression, and help you return to an active life.
2. Is it safe to do gym workouts or yoga with spinal degeneration?
Answer: It is safe if you practice correctly. You should prioritize exercises that strengthen your core muscles and avoid excessive bending, arching, or twisting of the spine. It is best to consult with and be supervised by a physiotherapist or an experienced trainer.
3. Should I use a back/neck brace?
Answer: Braces can be helpful during the acute pain phase to offload the spine, but they should only be used for a short period (less than 2 weeks). Overusing a brace can weaken your muscles and lead to dependency.
4. When is a spinal MRI needed, and when is surgery necessary?
Answer: A spinal MRI is necessary when there are red flags or when symptoms do not improve after more than 6 weeks of conservative treatment. Spinal surgery is indicated when there is evidence of severe nerve compression causing progressive weakness or debilitating pain that severely limits function.
5. What are the best sleeping positions and choices for mattresses/pillows?
Answer: You should sleep on your side with a pillow between your knees, or on your back with a pillow under your knees. Choose a medium-firm mattress (not too soft, not too hard) and a pillow of the appropriate height to keep your cervical spine aligned with the rest of your spine.
Conclusion
Complications of spinal degeneration can lead to severe consequences, from chronic pain to disability. However, the good news is that most of these complications can be effectively managed and prevented if detected early and treated properly. The key lies in maintaining good posture, exercising regularly to strengthen core muscles, and following a structured treatment plan that prioritizes conservative methods.
Don’t let chronic back pain control your life. If you are experiencing pain that lasts longer than two weeks or have any unusual symptoms, take action today.
Related articles:
Contact for consultation
MAPLE INTERNATIONAL CO., LTD
Phone: 0705 100 100
Tax code: 0311948301
Date Range: 21 - 08 - 2012
Issued: Department of Planning and Investment of Ho Chi Minh City