Common Spinal Conditions: Causes and Early Warning Signs
Common Spinal Conditions are among the leading causes of back pain and reduced quality of life across all age groups. This category covers a wide range of problems — from spinal degeneration and disc herniation to scoliosis — all of which directly affect the structure and function of the spine. Understanding these conditions is an important first step toward building an effective treatment plan and taking proactive steps to protect your spinal health long term.
Chronic back pain does more than cause discomfort — it limits your mobility and can affect your work, your sleep, and your ability to carry out everyday activities. These conditions are particularly common among people who do heavy physical labor, office workers who spend long hours sitting, and adults between the ages of 30 and 50.
This article provides a comprehensive overview of the most common spinal conditions, exploring their causes, symptoms, diagnostic approaches, treatment options, and practical advice to help you support the health of your spine.
Overview of Common Spinal Conditions
To understand spinal conditions, it helps to first understand how the spine is structured. The human spine consists of 33 vertebrae stacked on top of one another, divided into five regions: cervical (neck), thoracic (mid-back), lumbar (lower back), sacral, and coccygeal. Between the vertebrae sit intervertebral discs, which act as shock absorbers. The entire system is supported by joints, ligaments, and muscles, while also protecting the spinal cord and nerve roots running through it. The spine serves three primary functions: supporting the body’s weight, enabling flexible movement, and protecting the central nervous system.
Common Spinal Conditions is a broad term referring to disorders that disrupt this structure and function — whether through degeneration, injury, inflammation, or structural deformity. As a result, people with these conditions may experience pain, numbness, muscle weakness, and restricted movement.
The most frequently seen spinal conditions include:
- Spinal Degeneration: The natural wear-and-tear process affecting spinal cartilage and intervertebral discs over time. As cartilage breaks down, vertebrae may begin to rub against each other, causing pain, stiffness, and a grinding sensation with movement.
- Disc Herniation: This occurs when the soft inner nucleus of an intervertebral disc pushes through its outer fibrous ring and presses on nearby nerve roots or the spinal cord. It typically causes sharp, radiating pain that travels through the buttock and down the leg (sciatica), often accompanied by numbness and muscle weakness.
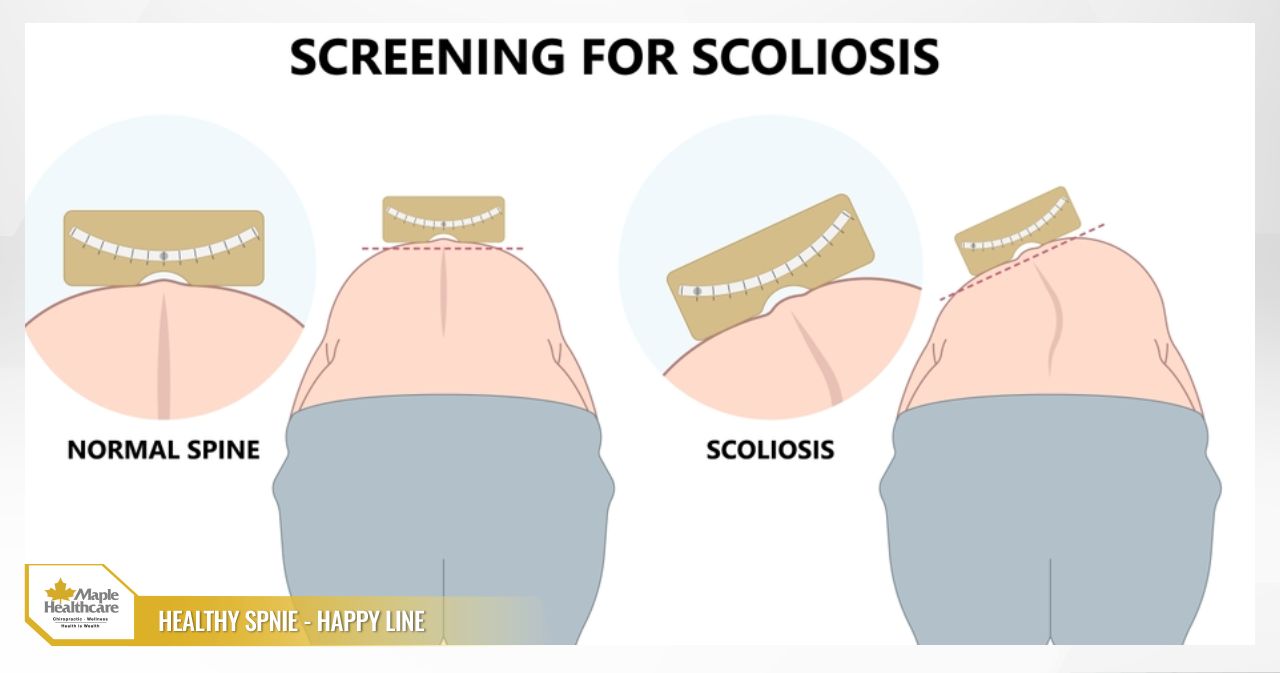
- Scoliosis: An abnormal lateral curvature of the spine. Scoliosis is typically diagnosed when the spinal curve (measured by the Cobb angle) exceeds 10 degrees. It can cause visible asymmetry in the shoulders and hips, and in more severe cases may affect respiratory function.
- Ankylosing Spondylitis: A chronic inflammatory condition primarily affecting the spinal joints. It causes pain and stiffness — especially in the morning or after periods of inactivity. Over time, vertebrae may fuse together, progressively reducing spinal flexibility. It most commonly affects young men between the ages of 15 and 30.
- Bone Spurs (Osteophytes): Bony growths that form along the vertebral bodies or spinal joints. These spurs can irritate surrounding soft tissue or compress nearby nerves, leading to localized pain.
- Sciatica: Pain that travels along the path of the sciatic nerve, from the lower back through the buttock and down the back of the leg. The most common underlying cause is a lumbar disc herniation pressing on a nerve root.
- Mechanical Back Pain: The most common form of back pain, typically caused by muscle spasm, muscle strain, or ligament sprain. Contributing factors include poor posture, improper lifting technique, and physical overexertion.
These conditions not only cause physical discomfort but can significantly impact daily life — reducing work productivity, disrupting sleep, and making routine activities such as sitting, bending, or carrying objects more difficult. Recognizing the signs early makes a meaningful difference in how manageable the condition becomes.
Causes of Common Spinal Conditions
Spinal conditions typically develop from a combination of factors rather than a single cause. Understanding these contributing factors can help guide both prevention and treatment.
Mechanical Factors and Degeneration
This is among the most significant groups of causes. Over time, intervertebral discs naturally lose moisture and elasticity, and their outer fibrous rings can develop small tears — leading to disc bulging or herniation. The cartilage in the facet joints also gradually wears down, resulting in degeneration, pain, and stiffness. While age-related degeneration is a natural process, several other factors can accelerate its progression.
Overload and Poor Posture
Everyday habits have a significant impact on spinal health:
- Improper lifting: Lifting heavy objects with the back rather than the legs places enormous pressure on the lumbar spine.
- Prolonged sitting with poor posture: Spending hours at a desk with a rounded back and a forward head position places continuous strain on the muscles and ligaments, contributing to mechanical back pain.
- Repetitive movements: Repeated bending and twisting — whether in occupational tasks or sports — can gradually damage the discs and surrounding structures.
Genetic and Immune Factors
Some spinal conditions have a recognized genetic component. Ankylosing spondylitis, for example, is strongly associated with the HLA-B27 gene. Idiopathic scoliosis is also thought to have a familial tendency.
Lifestyle and Environmental Factors
Certain lifestyle habits also play an important role:
- Physical inactivity: A sedentary lifestyle weakens the core muscles — the abdominal and back muscles that support and stabilize the spine.
- Excess weight and obesity: Carrying extra body weight increases the load on the spine — particularly the lumbar region — and can accelerate degenerative changes.
- Smoking: Nicotine reduces blood flow to the intervertebral discs, impairing the disc’s ability to receive nutrients and repair itself — contributing to earlier degeneration.
- Occupation: Jobs that involve heavy lifting, repetitive physical strain, or prolonged vibration (such as driving or construction work) carry a higher risk of spinal problems.
Identifying these causes and risk factors early is important to help prevent the condition from progressing to serious complications — including structural deformity, significant nerve compression causing weakness or paralysis, or in severe cases, long-term disability.
Symptoms of Spinal Conditions to Watch For
Symptoms vary widely depending on the type of condition and its severity. Paying attention to how your body feels and recognizing early warning signs can help you seek care at the right time.
Common Symptoms
- Back pain: The most frequent symptom. Pain may range from a dull ache to sharp, intense discomfort. It often worsens with activity, prolonged standing or sitting, and tends to ease with rest. In people with spinal degeneration, a grinding or clicking sensation during movement may also be present.
- Radiating nerve pain: A hallmark sign of disc herniation or spinal stenosis with nerve compression. Pain typically originates in the lower back, travels through the buttock and back of the thigh, and may extend to the calf and foot. This is often accompanied by numbness, a tingling or pins-and-needles sensation, or weakness in the leg.
- Morning stiffness: People with ankylosing spondylitis often experience significant pain and stiffness in the lower back upon waking that lasts more than 30 minutes. This typically improves once the person begins moving around.
- Visible spinal deformity: In scoliosis, noticeable asymmetry may be visible — such as uneven shoulder heights, one hip sitting higher than the other, or a rib hump that becomes apparent when bending forward.
These symptoms affect more than just physical comfort — they can make sitting for extended periods, bending, lifting, or even walking more difficult, reducing both productivity and sleep quality.
Warning Signs That Require Prompt Medical Attention
You should seek specialist care promptly if you experience any of the following, as they may indicate a serious underlying condition:
- Severe, persistent pain that does not ease with rest.
- Pain radiating below the knee, particularly if accompanied by numbness or leg weakness.
- Loss of sensation in the groin or around the anal region.
- Bladder or bowel dysfunction (urinary retention or incontinence).
- Noticeable weakness in one or both legs that affects your ability to walk.
- Fever or unexplained weight loss alongside back pain.
These are important warning signals that may indicate serious nerve damage or other conditions requiring urgent evaluation — such as spinal infection, spinal tuberculosis, or a tumor.
Diagnosis and Treatment of Common Spinal Conditions
Effective treatment begins with an accurate diagnosis. The diagnostic process typically involves several steps working together to build a clear clinical picture.
The Diagnostic Process
- Clinical examination: Your clinician will begin by taking a thorough history — asking about the location and character of your pain (dull, sharp, or stabbing), what makes it better or worse, and any associated neurological symptoms such as numbness or weakness. A physical examination follows to assess posture, range of spinal motion, muscle strength, sensation, and deep tendon reflexes. Specific orthopedic tests — such as the straight leg raise — may also be performed to check for signs of nerve root compression.
- Imaging studies:
- X-ray: A foundational tool for evaluating bony structures and spinal alignment, and for identifying bone spurs, narrowed joint spaces, vertebral slippage (spondylolisthesis), or structural deformity.
- MRI (Magnetic Resonance Imaging): Considered the gold standard for assessing soft tissue. MRI provides detailed images of the intervertebral discs, spinal cord, and nerve roots — enabling precise identification of disc herniation, the degree of nerve compression, and inflammatory changes.
- CT Scan: Typically ordered when more detailed evaluation of bony structures is needed, particularly in complex trauma cases.
Treatment Options
At Maple Healthcare in Ho Chi Minh City, the clinical team prioritizes conservative, non-surgical approaches that aim to address key underlying mechanical factors and support the body’s natural recovery.
Conservative (Non-Surgical) Treatment: This is the preferred first-line approach for the majority of patients.
- Chiropractic Care: Specialist clinicians use gentle, hands-on spinal adjustment techniques to address vertebral misalignments, help reduce pressure on affected nerves, and support improvements in pain and movement function.
- Physiotherapy and Rehabilitation: An individualized program incorporating stretching and targeted strengthening exercises for the back and core muscles — helping to improve spinal stability. Supportive modalities such as therapeutic ultrasound, electrotherapy, and heat therapy may also be incorporated to help manage pain and support tissue healing.
- Activity Modification: During the acute phase, some relative rest may be appropriate — however, prolonged bed rest is generally discouraged. Returning to gentle activity early, under clinical guidance, tends to support a faster and more complete recovery.
A personalized treatment plan that combines multiple approaches and is closely monitored by a multidisciplinary team is a key part of achieving meaningful improvement and reducing the risk of recurrence.
Prevention and Lifestyle Advice for Spinal Health
Prevention is always preferable to treatment. Building consistent healthy habits into your daily routine is one of the most effective ways to protect your spine and reduce your risk of developing these conditions.
Maintaining Good Posture and Ergonomics
- When sitting:
- Keep your back straight and supported by the backrest. A small lumbar cushion can help maintain the natural curve of your lower back.
- Adjust your chair height so your hips and knees are at roughly a right angle, with both feet resting flat on the floor.
- Position your computer screen at eye level, with your keyboard and mouse placed so your elbows bend at approximately 90 degrees.
- Most importantly: stand up, walk around, and stretch for a few minutes every 30 to 45 minutes of sitting.
- When standing and lifting:
- If you need to stand for extended periods, shift your weight between legs regularly.
- When lifting something heavy, always keep your back straight, bend at the knees and hips to lower yourself toward the object, hold it close to your body, and use the strength of your legs to lift — never round your back to pick something up. Avoid twisting your torso while carrying a load.
Regular Exercise and Physical Activity
- Stay consistently active: The World Health Organization recommends at least 150 minutes of moderate-intensity aerobic activity per week (such as brisk walking, cycling, or swimming), combined with two to three sessions of muscle-strengthening exercise.
- Exercises that support spinal health:
- Plank: Builds core muscle strength to support the spine.
- Bird-dog: Improves spinal stability and balance.
- Glute bridge: Strengthens the glutes and lower back muscles.
- Cat-cow stretch: Promotes spinal flexibility and mobility.
- Swimming and yoga: Excellent low-impact options that stretch and strengthen the whole body without placing excess load on the joints.
- Maintain a healthy weight: Keeping your weight within a healthy range helps reduce unnecessary load on the spine and intervertebral discs.
Nutrition and Other Healthy Habits
- Eat a balanced diet: Ensure adequate intake of calcium and vitamin D to support strong, healthy bones.
- Avoid smoking: Quitting smoking is one of the most beneficial things you can do for your long-term spinal health.
- Limit alcohol consumption: Excessive alcohol intake is associated with an increased risk of osteoporosis.
- Schedule regular check-ups: If you have a family history of spinal conditions or work in a physically demanding role, periodic spinal health assessments can help identify problems early.
Living with a Spinal Condition: Challenges and Strategies
Managing a chronic spinal condition can be a demanding experience. Persistent pain affects not only your physical health but also your mental well-being, your work, and your relationships. However, there are many practical strategies that can help you keep your condition under better control and maintain an active life.
Common Challenges
- Ongoing pain that can be difficult to manage day to day.
- Reduced mobility and difficulty participating in activities you enjoy.
- Disrupted sleep, leading to fatigue and irritability.
- Psychological impact, which may include anxiety or low mood over time.
Practical Coping Strategies
- Stay consistent with your rehabilitation program: Don’t stop your exercises once the pain subsides. Continuing the home exercise program recommended by your clinician is important for maintaining progress and reducing the risk of recurrence.
- Use supportive tools: An ergonomic chair, a lumbar support cushion for car journeys, or a suitable mattress can make a meaningful difference to your comfort. A back brace may be helpful for short periods during heavy tasks, but should not be relied on as a long-term solution.
- Manage pain thoughtfully: Learn to use heat therapy (warm compress) to relax tight muscles and cold therapy (ice pack) to help reduce inflammation. Listen to your body and pace your activities to avoid overexertion.
- Look after your mental health: Don’t hesitate to reach out for support from family, friends, or a mental health professional if you are feeling overwhelmed or persistently low.
Above all, taking an active role in your own care makes a real difference. If your symptoms are not improving or you notice any of the neurological warning signs described earlier, please seek assessment from a clinician or physiotherapist promptly.
Conclusion
Common Spinal Conditions — including spinal degeneration, disc herniation, and scoliosis — are widespread health concerns that develop primarily through the natural aging process, lifestyle habits, and genetic factors. While they can cause significant pain and functional limitations, the good news is that most cases can be managed effectively through conservative, non-surgical treatment approaches.
The keys to better spinal health lie in recognizing symptoms early, obtaining an accurate diagnosis, and following a personalized treatment plan. Equally important is a sustained commitment to lifestyle changes — maintaining good posture, exercising regularly, and eating a balanced diet.
Don’t let back pain limit what you can do. Start applying the advice in this article today. If you are experiencing persistent or unusual symptoms, consider booking a spinal assessment with the clinical team at Maple Healthcare for an evaluation and a personalized treatment plan — to help you move more freely and live more comfortably.
FAQ: Common Questions About Spinal Conditions
What are the main causes of spinal conditions?
Answer: The primary contributing factors include the natural degenerative changes that come with age, poor posture during daily activities and work (such as prolonged sitting or improper lifting), physical inactivity, excess body weight, and genetic predisposition in certain conditions such as ankylosing spondylitis.
When should I see a doctor for back pain?
Answer: You should seek medical care promptly if your back pain is severe and does not ease with rest, if it radiates into your leg with associated numbness or weakness, or if you experience more serious signs such as loss of bladder or bowel control, fever, or unexplained weight loss.
Can spinal conditions be completely cured?
Answer: Many spinal conditions — particularly those related to degeneration — are chronic in nature. However, symptoms can often be well controlled through conservative approaches such as chiropractic care and physiotherapy, helping many patients return to normal daily activities without the need for surgery. The goal of treatment is to reduce pain, improve function, and limit the risk of further complications.
Is prolonged sitting a major cause of common spinal conditions?
Answer: Yes — prolonged sitting, especially with poor posture, is one of the most significant risk factors. It places sustained pressure on the intervertebral discs, weakens the back and core muscles, and contributes to both mechanical back pain and the acceleration of spinal degeneration. Maintaining good posture and taking regular movement breaks throughout the day are important steps in reducing this risk.
Related articles:
Contact for consultation
MAPLE INTERNATIONAL CO., LTD
Phone: 0705 100 100
Tax code: 0311948301
Date Range: 21 - 08 - 2012
Issued: Department of Planning and Investment of Ho Chi Minh City