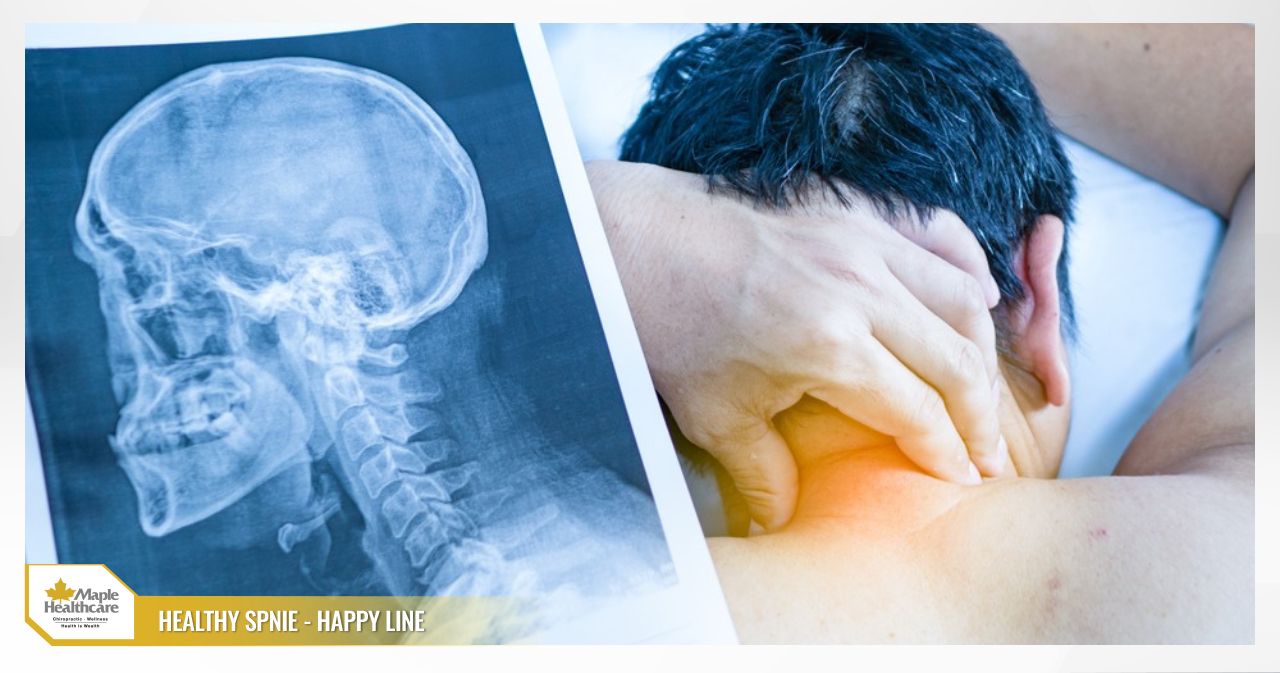
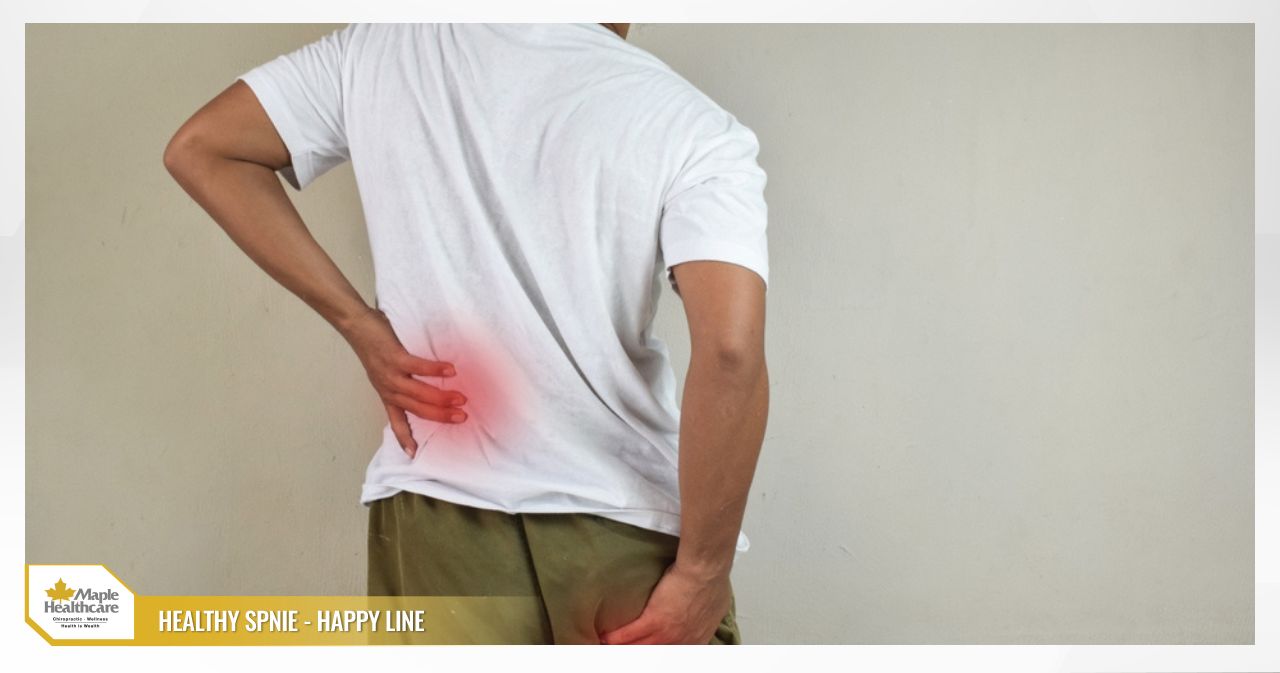
What Is Spinal Degeneration? Causes, Symptoms, and Treatment Options
Do you often experience neck, shoulder, or lower back discomfort after a long day of work? Persistent aches and morning stiffness can be early signs of Spinal Degeneration. This condition represents the natural aging process of bones, cartilage, and intervertebral discs. While very common in older adults, it is increasingly seen in younger people. Although many cases show no obvious symptoms, understanding this condition is key to managing pain and maintaining an active lifestyle.
This article will help you recognize the early symptoms of spinal degeneration, understand treatment options ranging from conservative care to surgery, and—most importantly—offer exercises and lifestyle changes to slow progression. Whether you are an office worker facing your first neck pain or back pain, a senior wanting to improve mobility, or an athlete looking to protect your spine, the information here will be valuable.
What Is Spinal Degeneration and Where Does It Commonly Occur?
Spinal degeneration is a general term describing the natural wearing down of spinal structures over time. This process affects the intervertebral discs, vertebral bodies, small facet joints, and ligaments, leading to pain, stiffness, and reduced mobility. In some cases, these changes can compress nerve roots or the spinal cord.
The disease mechanism progresses through several stages:
- Disc degeneration: The discs, which act as shock absorbers between vertebrae, lose water content and elasticity with age. The outer fibrous ring can crack or tear, allowing inner gel-like material to leak, causing disc herniation.
- Bone spur formation (Osteophytes): When discs collapse, the body responds by growing small bony projections (bone spurs) at vertebral edges to increase stability. These spurs can press on nearby nerves.
- Ligament thickening and fibrosis: Longitudinal ligaments along the spine become thicker and stiffer, losing flexibility and contributing to spinal canal narrowing.
- Facet joint arthritis: The cartilage covering the small joints at the back of the spine wears down, causing friction, inflammation, and pain on both sides.
Common locations of degeneration:
- Cervical spondylosis: The neck supports and rotates the head continuously, making it prone to degeneration, resulting in neck and shoulder pain that may radiate to the arms.
- Lumbar spondylosis: This is the most common area because it bears most of the body’s weight. Pain typically occurs in the lower back.
- Thoracic spondylosis: Less common because this part of the spine is supported by the rib cage and moves less. Degeneration here often occurs alongside cervical or lumbar regions.
It is important to note that not everyone with degenerative changes on X-rays experiences pain. Many live with these changes symptom-free. Diagnosis becomes meaningful when pain, stiffness, or neurological signs impact your daily life.
Causes and Risk Factors of Spinal Degeneration
While spinal degeneration is part of natural aging, certain factors can accelerate its progression. Identifying these risks is the first step in prevention.
- Age: The main risk factor. Discs and joints lose water and wear down more as you get older.
- Occupation: Jobs involving prolonged sitting (office workers), heavy lifting, or continuous vibration exposure (drivers, construction workers) increase spinal stress.
- Poor posture: Habits like slouching or looking down at your phone for extended periods (“text neck” syndrome) put excessive pressure on the cervical and lumbar spine.
- Sedentary lifestyle: Lack of movement weakens core muscles supporting the spine, increasing load on discs and joints.
- Overweight and obesity: Excess body weight increases pressure on the lumbar spine, speeding up degeneration.
- Smoking: Nicotine reduces blood flow to the discs, causing them to dry out and deteriorate faster.
- Genetics: Family history of spinal degeneration increases your risk.
- Previous injuries: Trauma from accidents or sports can damage spine structures and trigger earlier degeneration.
Typical Symptoms of Spinal Degeneration
Symptoms vary depending on the location and severity. Common signs include persistent or episodic pain, morning stiffness, and limited range of motion. Pain often worsens with overuse and eases with rest.
Symptoms in the Neck Area
- Dull neck pain that can radiate to the shoulders, shoulder blades, and arms. Pain intensifies when bending, extending, or rotating the neck, sometimes even coughing or sneezing triggers sharp pain.
- Stiffness in the neck, especially in the morning after waking up.
- Numbness, tingling, or prickling sensations in the arms and hands if nerve roots are compressed.
- Some individuals may experience headaches, dizziness, or tinnitus.
- Lhermitte’s sign: An electric shock-like sensation running down the spine when bending the chin toward the chest.
Symptoms in the Lower Back
- Lower back pain that may radiate to the buttocks, back of the thighs, and calves.
- Sciatic pain: Sharp, numbness, or weakness tracing the path of the sciatic nerve from the lower back down to the foot.
- Morning stiffness and difficulty bending or straightening up.
- Pain may worsen at night, affecting sleep quality.
- In severe cases, leg weakness or bladder and bowel dysfunction may occur.
Signs of Spinal Degeneration That Require Immediate Medical Attention
Seek medical care immediately if your neck or back pain is accompanied by any of the following symptoms:
- Fever, unexplained weight loss.
- Loss of bladder or bowel control (incontinence).
- Rapidly progressing numbness or weakness in the legs.
- Severe night pain that does not improve with position changes.
- History of cancer, osteoporosis, long-term corticosteroid use, or recent major trauma.
Aggravating Factors and Poor Lifestyle Habits
Beyond underlying causes, daily lifestyle factors can worsen spinal degeneration.
- Repeated overloading: Repetitive bending, twisting, or improper heavy lifting wear down discs and joints. Learning proper lifting techniques—bending knees, keeping the back straight, and using leg and hip strength—is crucial.
- Stress and poor sleep: Psychological stress causes muscle tension, while lack of sleep hinders the body’s natural recovery.
- Smoking: As mentioned, smoking harms discs by reducing their repair capacity.
- Overweight and obesity: Each extra kilogram multiplies the pressure on your lumbar spine when walking, standing, or bending.
- Poor nutrition: A diet lacking essential minerals like calcium, magnesium, and adequate hydration weakens the musculoskeletal system. Since discs are about 80% water, dehydration reduces their elasticity.
Diagnostic Process for Spinal Degeneration
Accurate diagnosis combines medical history, physical examination, and imaging studies.
- Medical history: Your doctor will ask detailed questions about your pain’s location, onset, factors increasing or relieving it, radiation, and accompanying symptoms like numbness or weakness. Reporting any “red flag” symptoms is also important.
- Physical examination: The clinician observes your posture, checks neck and back range of motion, assesses muscle strength, reflexes, and performs specific tests for nerve root compression (e.g., straight leg raise test).
- Imaging studies:
- X-rays: The first-line imaging tool to detect bone spurs, disc space narrowing, or vertebral slippage.
- MRI (Magnetic Resonance Imaging): Provides detailed images of soft tissues such as discs, nerve roots, and spinal cord. MRI is the gold standard for diagnosing disc herniation or spinal canal narrowing.
- CT scan (Computed Tomography): Gives detailed bone images, useful in complex cases or after trauma.
- Blood tests: May be ordered if infection or malignancy is suspected as a cause of pain.
Early imaging is typically indicated when to see a doctor if you have neurological symptoms (numbness, weakness), after major trauma, or when considering interventions. For simple mechanical pain, your doctor may recommend close monitoring and conservative treatment first.
Differentiating Spinal Degeneration from Other Conditions
Back and neck pain can arise from many causes. Accurate differential diagnosis guides suitable treatment.
- Disc herniation: Usually starts suddenly after exertion (lifting, twisting). Characteristic nerve root pain radiates along the nerve path. MRI shows herniated disc compressing the nerve root.
- Spinal stenosis: Characterized by neurogenic claudication—leg pain and fatigue when walking, relieved by sitting or leaning forward.
- Spondylolisthesis: A vertebra slips forward over the one below, visible on X-rays.
- Myofascial pain: Localized muscle pain with trigger points, not following nerve distribution and without numbness or weakness.
Non-Surgical Treatment Methods for Spinal Degeneration
The good news is most spinal degeneration cases respond well to conservative treatments. At Maple Healthcare in Ho Chi Minh City, we prioritize a multimodal, non-drug, and non-surgical approach to address key underlying causes of pain.
Education and self-management: The first step is understanding your condition accurately. Avoid prolonged bed rest and maintain gentle physical activity. Movement improves blood flow and nourishes the discs. Physiotherapy and rehabilitation: This forms the treatment foundation. Specialists design personalized exercise programs to reduce pain and inflammation, strengthen core muscles (transverse abdominis, erector spinae), improve flexibility, and guide safe home exercises. Chiropractic care: Chiropractors use gentle, precise spinal adjustments to correct vertebral misalignments, relieve nerve compression, and restore normal spine function.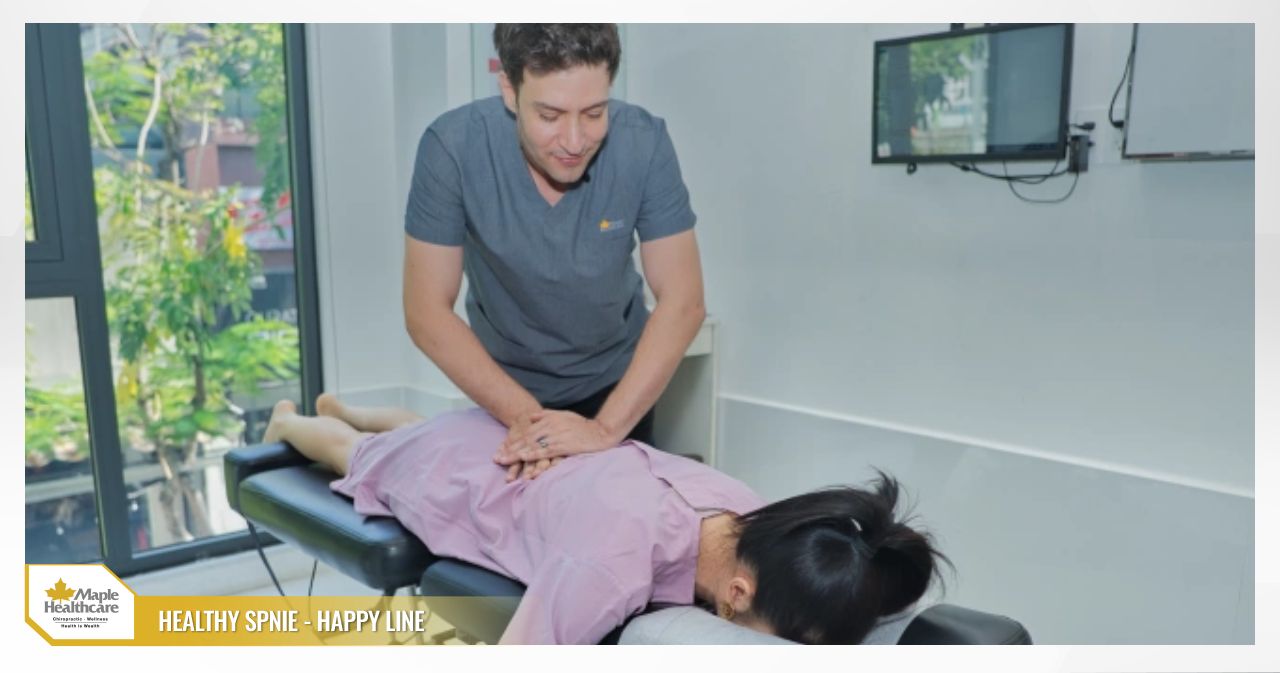 Medications (used under supervision): Common pain relievers (paracetamol), non-steroidal anti-inflammatory drugs (NSAIDs), and muscle relaxants may be used during flare-ups to control symptoms. Always take medications as prescribed to avoid side effects.
Supportive therapies: Heat/cold packs and therapeutic massage can provide temporary muscle pain relief. Use of neck braces or lumbar supports should be short-term (1-2 weeks) during acute pain episodes, to avoid muscle weakening from overuse.
Medications (used under supervision): Common pain relievers (paracetamol), non-steroidal anti-inflammatory drugs (NSAIDs), and muscle relaxants may be used during flare-ups to control symptoms. Always take medications as prescribed to avoid side effects.
Supportive therapies: Heat/cold packs and therapeutic massage can provide temporary muscle pain relief. Use of neck braces or lumbar supports should be short-term (1-2 weeks) during acute pain episodes, to avoid muscle weakening from overuse.
When Is Surgery Needed for Spinal Degeneration?
Spinal surgery is considered only if conservative treatments fail after a prolonged period (usually 3-6 months) and the patient presents with one or more of the following signs:
- Severe, persistent, and uncontrollable pain.
- Progressive weakness or paralysis in arms or legs.
- Severe spinal stenosis causing walking difficulties.
- Loss of bladder or bowel control (cauda equina syndrome)—a medical emergency.
Common surgical techniques include nerve decompression (removal of bone spurs or herniated disc material), spinal fusion, or artificial disc replacement.
Safe and Effective Exercises for Spinal Degeneration
Proper exercise is key for managing spinal degeneration. Always start gently, listen to your body, and stop if pain increases.
Exercises for Cervical Spondylosis
Chin Tucks: Sit or stand tall, looking forward. Gently retract your chin as if creating a double chin. Hold for 5 seconds, then relax. Repeat 10-15 times, twice daily. This activates deep neck muscles and improves head posture. Trapezius Stretch: Sit upright, place your right hand over your head onto the left ear, and gently tilt your head to the right until you feel a mild stretch on the left neck side. Hold for 20-30 seconds. Switch sides, repeat 2-3 times each.Exercises for Lumbar Spondylosis
Cat-Camel Stretch: Kneel on all fours. Inhale, arch your back downward and lift your head (Cow pose). Exhale, round your back upward and lower your head (Cat pose). Repeat 10 times, once or twice daily to improve spine flexibility. Bird-Dog: Start on hands and knees. Slowly extend your right arm forward and left leg backward, keeping your back and hips stable. Hold 3-5 seconds, then return. Switch sides. Repeat 10 times each to strengthen core muscles. Glute Bridge: Lie on your back with knees bent and feet flat on the floor. Tighten your glutes and slowly lift hips off the floor. Hold 2-3 seconds, then lower down. Repeat 15-20 times to strengthen glute muscles and reduce lower back load. Hip Hinge: Stand with feet shoulder-width apart. Keeping your back straight, push your hips backward and bend forward until you feel a mild stretch in the back of your thighs. This teaches proper bending and lifting techniques protecting your back.
Lifestyle, Proper Posture, and Preventive Measures
Prevention is better than cure. Adjusting daily habits has a significant impact on your spine health.
- Ergonomics at work: Adjust your computer screen to eye level. Use a chair with back support. Stand up and move around every 30–60 minutes.
- Proper lifting techniques: Always bend knees, keep your back straight, and hold objects close to your body. Use leg strength, not your back.
- Sleeping posture: Sleep on your back with a pillow under your knees or on your side with a pillow between your knees. Avoid sleeping on your stomach. Choose a mattress and pillow with medium firmness.
- Avoid “Text Neck”: When using your phone, try to raise it to eye level instead of bending your head downward.
- Maintain healthy weight and quit smoking: These two factors significantly reduce spinal load and improve nutrition.
Nutrition for Healthy Bones and Spine
A balanced nutritional diet for joints and bones plays an important supportive role in slowing degeneration.
- Anti-inflammatory diet: Increase foods rich in Omega-3 (salmon, walnuts), leafy greens, and fruits. Spices like turmeric (curcumin) and ginger also have anti-inflammatory effects.
- Essential micronutrients: Ensure adequate calcium, vitamin D, magnesium, and vitamin K2 intake. Drink enough water (2–3 liters per day) to keep discs hydrated and elastic.
- Supplements: Glucosamine Chondroitin and type II collagen may support cartilage structure; consistent use is needed to assess benefits.
- Foods to limit: Reduce refined sugars, processed foods, and alcohol as they can promote inflammation.
Complications and Prognosis
If not managed properly, spinal degeneration can lead to complications negatively affecting quality of life.
- Chronic pain: Persistent pain can interfere with daily activities, mood, and sleep.
- Spinal canal narrowing: Thickened ligaments and bone spur growth may narrow the spinal canal, compressing the spinal cord and nerve roots.
- Muscle weakness and numbness: Prolonged nerve compression can cause permanent muscle weakness and reduced mobility.
However, the prognosis for most cases is very good. With adherence to treatment plans, lifestyle changes, and regular exercise, most patients can control symptoms well and maintain an active life.
When to Seek Emergency Care?
You need urgent medical attention if you experience any “red flag” symptoms. Early diagnosis and intervention are extremely important.
- Loss of bowel or bladder control.
- Sudden, rapidly worsening weakness or paralysis in the legs or arms.
- Severe pain following major trauma (fall, accident).
- Pain accompanied by high fever and chills.
If you have any of these signs, do not hesitate to go to the hospital or specialist clinic immediately. These represent situations when to seek emergency care to prevent irreversible nerve damage.
Spinal degeneration is a long journey, but it is manageable. The key to success lies in early recognition, following a multimodal treatment approach, maintaining physical activity, and optimizing lifestyle and nutrition. Don’t let pain control your life.
Start today by trying 3-5 of the exercises listed above, adjusting your sitting posture at work, and paying closer attention to your body’s signals. If your pain does not improve after 4–6 weeks, or if you have any red flag symptoms, schedule an appointment with clinicians at Maple Healthcare in Ho Chi Minh City. We will conduct a thorough examination and create a personalized treatment plan combining chiropractic care and physiotherapy to help you safely and effectively return to an active life.
FAQ: Frequently Asked Questions About Spinal Degeneration
1. Can spinal degeneration be completely cured?
Answer: Degeneration is a natural aging process that cannot be fully reversed. However, treatment aims to control symptoms, improve function, and slow disease progression. With the right care, you can live a healthy life without being burdened by pain.
2. Should I get an MRI immediately when I have back pain?
Answer: Not always. MRI is usually recommended when neurological symptoms (numbness, weakness) occur, pain does not respond to conservative treatment, or when serious causes are suspected. Your doctor will decide the appropriate timing.
3. Is it good to wear a back or neck brace daily?
Answer: Not recommended. Continuous use of a back brace or neck collar can weaken the natural supporting muscles of your spine. These supports should only be worn short-term (1–2 weeks) during acute pain or for specific support.
4. Can people with spinal degeneration swim or practice yoga?
Answer: Yes, these are excellent sports choices. Swimming reduces pressure on the spine, while yoga improves flexibility and strength. However, choose appropriate classes and avoid excessive back bending or arching. Always discuss your condition with a coach or spinal physiotherapy expert.
Related Articles:
Contact for consultation
MAPLE INTERNATIONAL CO., LTD
Phone: 0705 100 100
Tax code: 0311948301
Date Range: 21 - 08 - 2012
Issued: Department of Planning and Investment of Ho Chi Minh City